There is an intimate connection between the body and the brain.
Dr. Stephen Porges, the originator of the Polyvagal Theory, identified a biological order of human response that is active in all human experience. Deb Dana, has brought the Polyvagal Theory to the world in a user-friendly format. I’ve written a few times about the role of the autonomic nervous system (ANS) in balancing the expenditure and conservation of our body’s energy. It is our own surveillance system, always checking if our environment is safe. This surveillance is happening at an unconscious level, outside the level of conscious thinking, and Dr. Porges coined the term neuroception to describe this phenomenon.
The ANS is made up of two branches, the sympathetic and parasympathetic. The sympathetic branch is in the spinal cord. It gets us ready for action, sending blood to muscles and increasing our heart rate and blood pressure. We are scanning for danger and preparing for fight or flight. In this state we can experience panic attacks, irritability, the inability to focus and to complete tasks, and the world doesn’t feel safe.
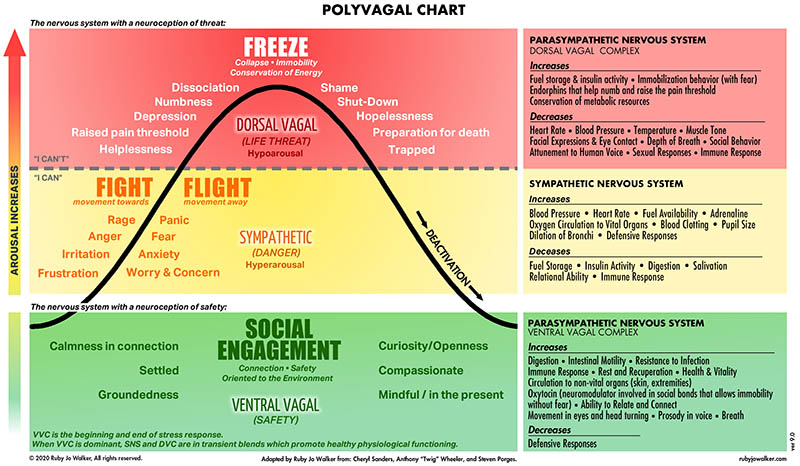
The parasympathetic branch is the home of the vagus nerve, which is divided into two parts: the ventral vagal pathway and the dorsal vagal pathway. The vagus runs upwards from the brain stem to connect with nerves in the neck, throat, eyes and ears and downwards into the lungs, heart and diaphragm and stomach.
The ventral vagal is our rest and digest or social engagement pathway. It is the most recent pathway to develop and is unique to mammals. When we’re in this state we feel safe and connected to others, our heart rate and breathing are regulated and we can experience joy and a sense of well being.
The dorsal vagal pathway is the freeze response and in this state we feel trapped and overwhelmed, disconnected or numb and go into collapse. We can feel alone, abandoned and too tired to think or act.

Deb Dana uses the analogy of a ladder to describe the three pathways, with the ventral vagal at the top, the sympathetic system in the middle and the dorsal vagal at the bottom. Our desired spot is at the top of the ladder where we feel connected to ourselves and others. Moving into the sympathetic system is protective at times, for instance, it mobilizes our body and mind to brake quickly if a car suddenly swerves into our lane. Once we’re out of danger, there has been no collision, and traffic is moving normally, our heart rate slows and within a few minutes we’ve forgotten about the incident and moved back up to the ventral vagal state. If, however, our heart keeps beating fast, we can’t get the incident out of our mind and we’re still reliving it in our mind when we get to our destination, we’re now staying in the sympathetic state and on alert for further danger. If we’re so distressed by the incident we can’t continue to our destination and instead have to head home and lie down and feel disconnected from those at home, we’ve now entered the dorsal vagal state and it’s a longer climb up the ladder.

One of the best methods to begin moving back up the ladder is using the breath to start bringing regulation to the nervous system. The in breath increases heart rate and the out breath brings the heart rate down and calms the nervous system. Therefore, taking short in breath’s and long, slow out breath’s begins to bring the nervous system back into balance and allows for movement up the ladder. When in the sympathetic or dorsal vagal response, focusing on breathing isn’t always easy. Having cues to remind you to breath or inviting a family member or friend to remind you to use the breath in difficult moments may be helpful.
When the nervous system is stuck in the sympathetic or dorsal vagal state, NeurOptimal® Neurofeedback interrupts that electrical pattern over and over during the training. Gradually the system comes back into balance so that moving back up the ladder becomes easier and easier.
